The Timed up and Go test is a mobile-native test for iOS and Android widely used for balance assessments in patients. It is often used to assess older patients’ risk of falling. It can be executed on the Qolty platform as a module in your study, either at home or in the clinic. See the information below to view how the TGUG works.
The timed-get-up-and-go task is a widely used test to determine balance assessment. Many parameters are developed and devised to determine a patient’s balance assessment. Most of the screening tools are developed to determine older patients’ risk of falling. The Timed-Get-Up-and-Go (TUG) test is a modified version of the Get-up-and-Go (GUG) which was initially developed by Mathias et al. 1986. The “Get-up-and-Go” (GUG) relied on subjective measurement because the performance was rated on a 5-point scale where 1 was normal, and 5 was strictly abnormal with a higher risk of falling. In this version, an individual rises from a chair, walks at a 3-meter distance, turns around, returns, and sits back on the chair.
To improve and change the subjectivity of the “Get-up-and-Go” (GUG) test, it was modified by the inclusion of time measurement for the entire procedure. The use of a chair and stopwatch with a 3-meter walkway is necessary to perform the task. The entire procedure from standing up, walking, turning around, and then going back to the chair was timed. It was observed that older adults who finished the whole procedure in under 10 seconds had no balance deficiency while those who took more than 10 seconds had a high risk of falling.
In a more advanced version, the Expanded Timed Get-up-and-Go (ETGUG), all series of tasks such as seated position, walking, turning, stopping, and sitting down are measured separately using a multi-memory stopwatch as incorporated in the ConductScience Digital Health App. The assessment is usually scored automatically by the smartphone (Galán-Mercant et al. 2014). In ETGUG, intensive time measurement is followed with respect to the component tasks. This approach pinpoints the main area of the patient’s problem. Although TGUG is reliable in determining balance assessment among elderly patients, it is substantial to isolate the areas of functional deficit to provide useful clinical information.
A study on the timed get-up-and-go test is revisited by measuring its component tasks (Wall et al. 2000). The basic procedure for TGUG is modified with different walkway measurements and stopwatches to monitor different activities. The chair used has no armrest with a sea elevation of approximately 46 cm. The general procedure is as follows:
The use of a multimemory stopwatch which has lap buttons should be pressed at the following event:
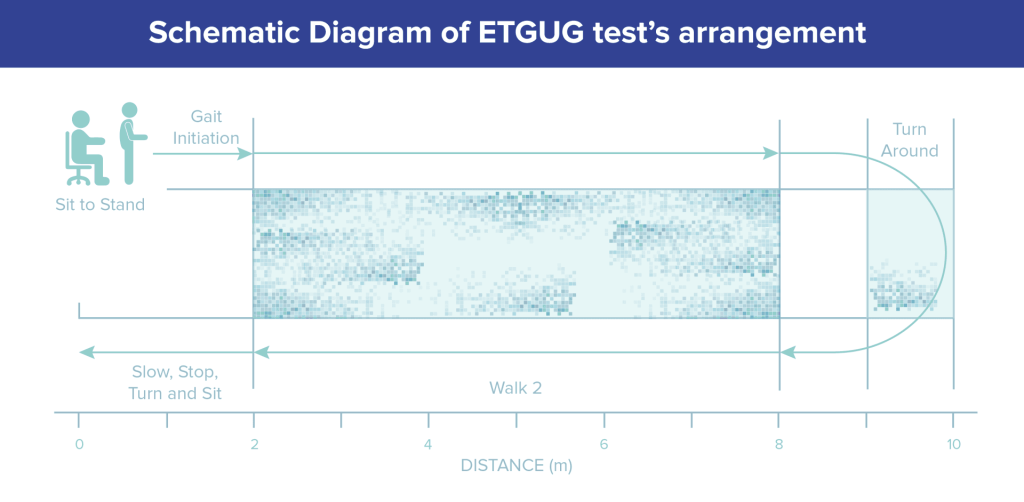
Figure 1. Schematic Diagram of ETGUG test’s arrangement
Both TGUG and ETGUG tests are performed among three groups such as healthy young individual, healthy elderly, and elderly who has a greater risk of falling.
Swanenburg et al. 2014 performed the timed-get-up-and-go test in patients with bilateral vestibular loss. The test was performed twice among 21 BVL patients and 21 controls aged 58±14 years old with two different recruiters. It was observed that BVL patients walked slower paralleled to control subjects. Therefore, ETGUG tests show good reliability for BVL patients with functional deficits.
Another study on timed get-up-and-go predicted an explanation of falls in elderly adults performing physical exercises (Virtuoso et al. 2014). Over a span of 12 months, data were collected for the participants with an occurrence of falling. It was observed that the classic and cognitive TUG tests have an indirect relationship with the manifestation of falls. This is due to a different factorial cause of falling during physical activity which can be intrinsic or extrinsic. The prediction should be assessed in a broad range within the protocols or elderly population.
Faria et al. 2012 performed the Expanded Timed Get-up-and-Go task on patients who had undergone stroke. In this study, intra and interrater reliabilities of the ETGUG test were validated and compared among patients who suffered a stroke and healthy individuals. It was observed that the group who suffered from stroke took a long time in every activity of the test.
A comparative study between left and right hemiplegics using ETGUG was performed by Muthukaruppan et al. 2011. Male individuals ages 45-55 who suffered from either left or right immobility were assessed. The time it took for each subject to perform different component tasks were recorded. It was observed that individuals with left hemiplegia took more time to stand up, turning, and sitting down while the individuals with right hemiplegia were having trouble with gait initiation, walking & speed.
A preliminary investigation of the efficacy of clinically practical dual-task tests as a concussion assessment tool was performed by Finer. 2014. 54 healthy individuals were subjected to a physical task; expanded time-get-up-and-go (ETGUG) and three cognitive activities such as backward digital recall (BDR), serial sevens (SS), and auditory pure switch task (APST). Finer concluded that the response rate of SS and APST was declined when combined with the ETGUG test. On the other hand, the response rate of BDR was comparatively enhanced when combined with ETGUG.
Bromboszcz et al. 2010 assessed ETGUG among patients with chronic obstructive pulmonary disease (COPD). In their study, a 20-meter walking distance was used for the test since it is the best metric to assess the walking abilities of patients. It emerged as a breakthrough because the typical testing for COPD such as 6MWT requires more walking distance.
The sample data represents the average time spent by healthy young, healthy adults, and at-risk adults to complete the entire course of the test. It is evident from Figure 2 that the time spent by the three groups is in the following order: At-risk adults > Adults > Young
Figure 2. TGUG and ETGUG test mean and standard deviation

The data for Figure 3, shows the time measured for each component in ETGUG test. It is observed that the at-risk control group took a long time to accomplish each task. Among all the components, Walk 1 shows significant differences among the three groups. While the young and elderly groups have a marginal difference, the at-risk group spent almost twice their time.

The timed-get-up-and-go task’s wide range of applicability makes it unique. It is a practical and reliable assessment tool to determine a patient’s balance assessment. It can be used by clinicians with great ease as it requires minimal equipment and professional skills.
This test screens functional deficiencies that help the clinician in designing more productive intervention strategies. It is a promising tool to determine a patient’s static and dynamic balance extensively. The specificity of the task is phenomenal as different components of balance assessment are evaluated rigorously.
Although widely used, but still further research is required to build a more robust correlation between increased component time and specific functional deficiency.
Bennie S, Bruner K, Dizon A, et al. Measurements of balance: comparison of the timed ‘Up and Go’ test reach test with the Berg Balance Scale. J Phys Ther Sci, 2003, 15: 93–97
Boonstra A., Stewart R., Köke A., Oosterwijk R., Swaan J., Schreurs K., Preuper H. (2016, September). Cut-Off Points for Mild, Moderate, and Severe Pain on the Numeric Rating Scale for Pain in Patients with Chronic Musculoskeletal Pain: Variability and Influence of Sex and Catastrophizing, 7: 1466, PMCID: PMC5043012
Botolsfen P., Helbostad J., Wall J. (2006, December). The modified Expanded Timed Get-Up and Go test reliability and concurrent validity, 24, 278-279
Bromboszcz J., Wloch T., (2010). Medical Rehabilitation. Tests of the functional performance of patients with COPD: A proposal for the application of the Expanded Timed ‘Get Up and Go Test’ (ETGUG). 14 (1), 22-34
Brooks TM., Mittermeier RA., da Fonseca GA., Gerlach J., Hoffmann M., Lamoreux JF., Mittermeier CG., Pilgrim JD., Rodrigues AS. (2006, July). Global Biodiversity Conservation Priorities. 313, 58-61, DOI: 10.1126/science.1127609
Brown T., Rutter L. (2015, January). Reliability and Validity of the Dimensional Features of Generalized Anxiety Disorder, 29: 1–6. DOI: 10.1016/j.janxdis.2014.10.003
Brusse KJ., Zimdars S., Zalewski KR., Steffen TM. (2005, February). Testing functional performance in people with Parkinson disease, 85(2), 134-41, PMID: 15679464
Caixeta, G. C. d. S., Doná, F., et al. (2012). Cognitive processing and body balance in elderly subjects with vestibular dysfunction. Brazilian Journal of Otorhinolaryngology 78(2): 87-95.
Clark M. S., Lemay E. P. , Jr (2010). “Close relationships,” in Handbook of Social Psychology 5th Edn Vol. 2 eds Fiske S. T., Gilbert D. T., Gardner L., editors. (Hoboken, NJ: John Wiley & Sons, Inc.) 898–940
Dal Bello-Haas V., Klassen L., Sheppard S., Metcalfe A. (2011, January). Psychometric Properties of Activity, Self-Efficacy, and Quality-of-Life Measures in Individuals with Parkinson Disease, 63(1), 47–57, DOI:10.3138/ptc.2009-08
de Morton, N. A., Berlowitz, D. J., et al. (2008). A systematic review of mobility instruments and their measurement properties for older acute medical patients. Health Qual Life Outcomes 6: 44
Faria C., Teixeira-Salmela L., Silve E., Nadeau S. (2012, June). Expanded Timed Up and Go Test with Subjects with Stroke: Reliability and Comparisons with Matched Healthy Controls, 93
Finer L., (2014, August). Preliminary investigation of the efficacy of clinically practical dual-task tests as a concussion assessment tool: a comparison of single-and dual-task tests on healthy young adults. University of Hawaii, Manoa.
Flansbjer UB., Holmbäck AM., Downham D., Patten., Lexell JC. (2005, March). Reliability of gait performance tests in men and women with hemiparesis after stroke, 37(2), 75-82, DOI: 10.1080/16501970410017215
Galán-Mercant A., Barón-López F., Labajos-Manzanares M., Cuesta-Var A. (2014, December). Reliability and criterion-related validity with a smartphone used in timed-up-and-go test, 13, 156. DOI: 10.1186/1475-925X-13-156
Gill-Body K., Beninato M., Krebs D. (2000). Relationship Among Balance Impairments, Functional Performance, and Disability in People With Peripheral Vestibular Hypofunction, 80 (8), 748-758, PubMed: 10911413
Huang SL., Hsieh CL., Wu RM., Tai CH., Lin CH., Lu WS. (2011, January). Minimal detectable change of the timed “up & go” test and the dynamic gait index in people with Parkinson disease, 91(1), 114-21, DOI: 10.2522/ptj.20090126
Katz-Leurer M., Rotem H., Lewitus H., Keren O., Meyer S. (2008, August). Relationship Between Balance Abilities and Gait Characteristics in Children With Post-Traumatic Brain Injury, 22 (2), 153-159, DOI: 10.1080/02699050801895399
Kennedy D., Stratford P., Wessel J., Gollish J., Penney D. (2005, January). Assessing stability and change of four performance measures: a longitudinal study evaluating outcome following total hip and knee arthroplasty, 6:3. DOI: 10.1186/1471-2474-6-3
Knorr S., Brouwer B., Garland SJ. (2010, June). Validity of the Community Balance and Mobility Scale in community-dwelling persons after stroke, 91(6), 890-6, DOI: 10.1016/j.apmr.2010.02.010
Maly M., Costigan P., Olney S. (2005, December). Contribution of Psychosocial and Mechanical Variables to Physical Performance Measures in Knee Osteoarthritis, 85 (12), 1318-1328, DOI: https://doi.org/10.1093/ptj/85.12.1318
Marchetti A., Felicioni L., Malatesta S., Grazia Sciarrotta M., Guetti L., Chella A., Viola P., Pullara C., Mucilli F., Buttitta F. (2011, September). Clinical features and outcome of patients with non-small-cell lung cancer harboring BRAF mutations, 29(26), 3574-9. DOI: 10.1200/JCO.2011.35.9638
Mathias, S., Nayak, U., et al. (1986). Balance in elderly patients: the” get-up and go” test.” Archives of physical medicine and rehabilitation, 67(6): 387
Meretta BM., Whitney SL., Marchetti GF., Sparto PJ., Muirhead RJ. (2006). The five times sit to stand test: responsiveness to change and concurrent validity in adults undergoing vestibular rehabilitation, 16(4-5), 233-43, PMID: 17538213
Morris, S., Morris, M. E., et al. (2001). Reliability of measurements obtained with the Timed “Up & Go” test in people with Parkinson disease. Physical Therapy 81(2): 810-818
Muthukaruppan S., (2011). A Comparative Study on Extended Timed Get Up and Go (ETGUG) Test Between Right and Left Hemiplegics. International Journal of Current and Review, 70-77
Nordin, E., Rosendahl, E., et al. (2006, May). Timed “Up & Go” test: reliability in older people dependent in activities of daily living–focus on cognitive state. Phys Ther 86(16649889): 646-655
Podsiadlo D., Richardson S. (1991, February) The timed “Up & Go”: a test of basic functional mobility for frail elderly persons, 39(2), 142-8. PMID: 1991946
Podsiadlo D., Richardson S. (1991, February). The timed “Up & Go”: a test of basic functional mobility for frail elderly persons; 39(2), 142-8, PMID: 1991946
Ries JD., Echternach JL., Nof L., Gagnon Blodgett M. (2009, June). Test-retest reliability and minimal detectable change scores for the timed “up & go” test, the six-minute walk test, and gait speed in people with Alzheimer disease. 89(6):569-79, DOI: 10.2522/ptj.20080258
Rockwood, K., Awalt, E., et al. (2000). Feasibility and measurement properties of the functional reach and the timed up and go tests in the Canadian study of health and aging. Journals of Gerontology. Series A, Biological Sciences and Medical Sciences 55(2): M70-73
Steffen A., Hagenah J., Graefe H., Mahlerwein M., Wollenberg B. (2007). Obstructive Sleep Apnea in Patients With Parkinson’s Disease–Report of Two Cases and Review, 87 (2), 107-111, DOI: 10.1055/s-2007-966889
Steffen TM. , Hacker TA, Mollinger L.(2002, February). Age- and gender-related test performance in community-dwelling elderly people: Six-Minute Walk Test, Berg Balance Scale, Timed Up & Go Test, and gait speeds, 82(2), 128-37. PMID: 11856064
Swanenburg J., Hegemann SC., Zurbrugg A., Palla A., de Bruin ED. (2014). Reliability and validity of the extended timed-get-up-and-go test in patients with bilateral vestibular loss, 34(4), 799-807. doi: 10.3233/NRE-141083
Van Hedel H., Wirz M., Dietz V. (2005, February). Assessing walking ability in subjects with spinal cord injury: Validity and reliability of 3 walking tests, 86(2), 190–196, DOI: http://dx.doi.org/10.1016/j.apmr.2004.02.010
Virtuoso J., Gregorio L., Merdeiros P., Mazo G. (2014). The “Timed Up and Go” in the prediction and explanation of falls in old people practicing physical exercise. 16(4), 381-389. DOI: 10.5007/1980-0037.2014v16n4p381
Wall J., Bell C., Campbell S., Davis J. (2000, February). The Timed Get-up-and-go Test Revisited: Measurement of the Component Tasks, 37(1), 109-114.
Whitney SL, Marchetti GF., Schade A., Wrisley DM. (2004). The sensitivity and specificity of the Timed “Up & Go” and the Dynamic Gait Index for self-reported falls in persons with vestibular disorders, 14(5), 397-409, PMID: 15598995
DISCLAIMER: ConductScience and affiliate products are NOT designed for human consumption, testing, or clinical utilization. They are designed for pre-clinical utilization only. Customers purchasing apparatus for the purposes of scientific research or veterinary care affirm adherence to applicable regulatory bodies for the country in which their research or care is conducted.